How Otis College's Dr. Julie Spencer Adapts Her Medical Practice for Artists and Designers
“I noticed really quickly at Otis that I couldn’t tell an art and design student, ‘Go and journal, or go and draw,’ [to deal with stress] because they’re already doing that stuff,” says Dr. Julie Spencer.

Dr. Julie Spencer in her office at Otis College’s Student Health and Wellness Center. Photo by Jennifer Atalla
Dr. Julie Spencer is as local as they come. Raised in Pasadena, California, she attended Loyola Marymount University just north of Otis College, and resides in Manhattan Beach, just south of the campus, with her husband and two children. She has dedicated her career to the care of teens and adolescents, starting with a subspecialty fellowship in Adolescent Medicine at Children’s Hospital Los Angeles, and continuing with founding and running Otis College’s Student Health and Wellness Center, the only of its kind on any AICAD (Association of Independent Colleges of Art & Design) campus. She also has a combined medical degree and Masters of Public Health from St. George’s University School of Medicine. Dr. Spencer’s MPH degree has uniquely qualified her to guide Otis through the COVID-19 pandemic, work that began with an early warning to the community about the threat of the virus in January 2019, long before it was a mainstay of nightly news telecasts. “When Otis College opened the doors to the new Student Health and Wellness Center in 2016, I would have never imagined how fortunate we were at that time to have hired Dr. Spencer,” says Laura Kiralla, the Vice President of Campus Life at Otis College. “Her double board-certification in pediatrics and adolescent medicine is a unique find in a higher education physician. She has led the College in managing the pandemic, supporting students every step of the way.”
We recently spoke with Dr. Spencer about what brought her to Otis, the unique challenges associated with treating art and design students, and the inherent rewards of working in such a creative environment.
What was the appeal of being a physician at an art and design college?
The biggest thing that attracted me was actually working with a college-age population. I’m double board-certified—my initial training is as a general pediatrician, and then I did additional training in adolescent and young adult medicine. I love working with college-age students. When this opportunity came up I was working at Kaiser in their teen clinic in Panorama City. I wasn't getting the experience with adolescents and young adults that I really wanted. So I was hired to help build the Student Health and Wellness Center at Otis and also to get to work with this population on a daily basis. I knew Otis from when I was a student at Loyola Marymount University. With Otis being an art and design school, I was very off-base when I came. I thought it wasn’t going to be a rigorous curriculum; I thought it was just going to be more studio-oriented work. I was very shocked, and very put in my place, with how rigorous Otis’s art and designed curriculum is. Coming from medicine, where everything is protocolized and procedure-based and sterile, I thought art and design school would be more free-flowing. But there’s definitely structure to getting a BFA, including a liberal arts education.
How do you adapt your practice for art and design students then?
Medical training for adolescents and young adults is very different from adult or just pediatric training, in the sense that with adolescents and young adults you have to use a psychosocial model of medicine. Something like abdominal pain is not just abdominal pain from a physical standpoint. You also have to consider, “OK, could this be depression? Could this be anxiety? Could this be something social like trouble with friends?” You have to add all of that into your differential diagnosis. I remember in my training being taught that for adolescents and young adults you have to try thinking outside the box for treatment ideas, so thinking, “Hey, do you like to journal? Do you like to draw or paint? Let’s talk about ways to get that anxiety or that depression out instead of internalizing it.” Internalizing is where we see physical ailments and physical symptoms start to manifest. I noticed really quickly at Otis that I couldn’t sit there and tell an art and design student, “Hey, go and journal, or go and draw,” because they’re already doing that stuff. I didn’t want to sit there and say, “Let’s get your self-expression out” when they’re already doing that as their day-to-day. I have to be really, really creative and that was something that was hard for me at first. It gets down to the fact that you can’t really protocolize art and design students. The treatment has to be very individualized. Obviously, if the problem is something that requires antibiotics, I’m giving a student antibiotics. But if it’s something that we need to go through the bio-psycho-social stuff, we then get down to individual ways that we can work through that. I’m not a counselor by any means, but my specialty in adolescents and young adults taught me about that psychological and social construct where, in my general pediatric training, I didn’t learn any of that. And this is the aspect of adolescent and young adult medicine that I love so much, that it has a counseling component to it. I get to really spend the time and get to know the student.
What are your interactions with students generally like? And do they see themselves as partners with you in their self-care?
Absolutely. Students are coming to Otis to get an education first and foremost, and our job is to ensure that they’re the healthiest that they can be to get that education. But part of our job is also to educate them on health for themselves, and to try to get them to come out of Otis and out of their experiences with us as good health consumers. So I’ll sit down and take that extra time with them. And it’s not just me, I teach my staff to take that extra time with students, and I’ve said to them, “Don’t just tell the student what they need to do, make sure they’re actually learning how to do it, because they don’t have their parents to rely on anymore.” They’re adults, and I never want to come across as if I’m talking down to a student. It’s more like, “Let’s have this equal conversation together and let’s be realistic.” You have to meet the students where they are. My interactions with students are on a personal, individual basis to educate them on their own health.
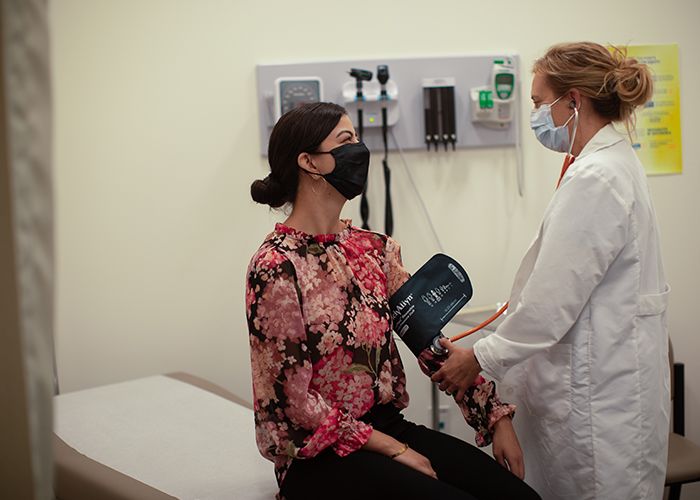
Dr. Spencer treating a student at the Student Health and Wellness Center at Otis College. Photo by Jennifer Atalla
How have you been able to come up with ways to help students keep their stressors from manifesting physically?
This is my sixth academic year at Otis, and throughout my time here I’ve learned some things. And even though I don’t want to give them more homework, it’s getting them to work with the medium that they have to get all of that stuff figured out. “Things that are bothering you, how does that look in your artwork? How you produce your artwork for an assignment is going to be a reflection of what you’re going through in that moment. How do you get your art to work for you?” is essentially what I try to say to them. It’s not just a blanketed prescription to go ahead and journal. I try to talk to them individually based on what they're working on, and then I’m always a big proponent of getting students moving, getting them physical. That is something that I see a lack of in art and design students because it’s just the nature of art and design—you’re sitting there, in front of a computer, or in front of an easel, but you’re sitting. I’m always talking to them about movement, and I’m not expecting them to go run miles. Just get the blood flowing. Not only is that going to help with their stressors, but it also helps to get the creative juices going.
How were you and your team at the SHWC able to mobilize when the COVID-19 pandemic was taking hold and impacting in-person instruction?
The pandemic was something that we were following very closely with the Centers for Disease Control and the L.A. County Department of Public Health, which we continue to do now. I’m on calls with the LACDPH every two weeks, specifically on guidelines for institutions of higher education. We’re constantly looking at what is changing. And with every stage of the pandemic we’ve been able to very quickly modify our process and work through what we need to do. The date that changed everything was spring break. We sat there and thought, “OK, it looks like students aren’t going to be able to come back on campus, how do we switch to continue offering healthcare?” The SHWC has always been open throughout this pandemic, we just very quickly mobilized to a telehealth operation. We were already using Zoom, and then we found out that Zoom developed a HIPAA-compliant telehealth platform, which we adopted because consent forms and consent for treatment for telehealth is very different than in-person. We had to figure out what telehealth meant for students that suddenly were in different states because me and my staff are all licensed in California. We had to quickly get into all of that, but we never shut our doors. We just changed our modality. Of course there are certain things that we cannot do over telehealth, so we sometimes screened students to come in, going through a COVID checklist. One thing that I am extremely proud of my department and staff for is that there was never a time that we told a student, “No, we’re not available to give you care.”
What was it about your medical training that prepared you for dealing with the pandemic?
Not only do I have my medical degree, but I also have an MPH, which is a Masters in Public Health. Dealing with a pandemic is right in my wheelhouse of what I studied and what I did for my masters degree. Also being well-versed in college health, where we see things like outbreaks in residential settings or in the college-wide campus, absolutely prepared me for this. Prior to the pandemic, we had a pertussis outbreak in the Residence Hall. I’ve joked that the pertussis outbreak was a mini, real-life preparation for the pandemic because I was working with the LACDPH on contact tracing and testing and we had to isolate students. But if you don’t have a full student health and wellness center on a campus, you don’t know what you need to look for when something like this happens.
What would you say to parents of students, or students themselves, who might have concerns about being back in the classroom right now?
I would say that the College is doing everything possible to ensure the health and safety of our students, and assure the parents of students, as well as faculty and staff, that it is our number one priority to follow all the guidance from the CDC and the LACDPH. We are not going outside of that. When the LACDPH said there were indoor mask mandates even if you’re vaccinated, boom, we were doing it. We’re following all the cleaning guidelines; we’re following all of the different mandates in real time. We are mandating COVID vaccines for our students and we have 97 percent of our students vaccinated, which is huge. They say that herd immunity happens for COVID at around 80 to 85 percent, so for our student population we’re definitely well above that. We’re mandating vaccines for our employees, which is very important as well. We are essentially trying to create as much of a health and safety bubble on our campus as possible. Of course, we don’t just live in a bubble. Students go off campus. They hang out with folks from LMU, or they see their families from Texas, etc. The next part is education and telling students that when they go off campus, to please make sure to wear a mask, wash your hands, and follow all of the guidance.
How would you generally characterize students’ feelings about the pandemic and their willingness to adhere to the guidelines set forth by the College with your input?
Generally, students have received the guidelines well. Obviously, we have some squeaky wheels out there. There have been some strong opinions regarding the mandate for the vaccine, but we have been meeting those students individually, and we are allowing for some exemptions. But generally as a whole students are very willing to adhere to the guidelines. Wearing masks has become the norm so we’re not having students really fight us on that. We're getting the sense that students are thinking not just of themselves, but of protecting “the Nest” at Otis, and protecting their fellow students, staff, and faculty.
What does it mean that Otis College is the only AICAD school that has an on-campus health and wellness facility with a full-time physician and nurses?
What that means is that we have met a certain set of standards for the Student Health and Wellness Center. There is a governing board or body called the AAAHC, which stands for the Accreditation Association for Ambulatory Health Care that has accredited our SHWC. We provide both medical and mental healthcare at a certain standard level. For all college student health centers, AAAHC is the gold standard. LMU’s student health center is AAAHC-accredited; USC’s is accredited. It means that we are providing a gold standard of care to our students. I commend Laura Kiralla, and I commend the senior administration, for acknowledging the importance of the Student Health and Wellness Center. If anything, this pandemic has reinforced how important it is for us to be on campus. If we were not here, where else would students be going to get their healthcare?

Dr. Spencer with Student Health and Wellness Center staff, from left: Kim Roark, SHWC Operations Manager; Bell Charkarutpahu, Registered Nurse; and Trisha Chiang, Family Nurse Practitioner. Photo by Jennifer Atalla
And finally, what do you love about working at an art and design college? Do you have any artistic tendencies, or has being surrounded by artists and designers had any sort of impact on you?
I get asked this question a lot by my outside peers. I would actually say that I love being surrounded by the creativity. Medicine can be very procedure-oriented, and very sterilized. They say that there’s an art to medicine, however, it is very different than an art and design environment. Annual Exhibition [the showcase of graduating student work across the College] is my favorite time of the year because we see students in such a different capacity. Ordinarily, we see students when they’re at their worst—when they’re sick, when they’re not feeling well, when they’re stressed out. And then when we see their work at Annual Exhibition, and students will run up to me and say, “Dr. Spencer, this is what I was working on that entire time you were helping me.” They’re so excited to share it with you and you’re so proud of them, and you see their creativity and it just blows your mind. In the Student Health and Wellness Center we have student artwork up and my ideal is to have a rotation of student artwork up because I love being able to support the students in that way. As for my own artistic tendencies, they are very minimal. I do love DIY stuff. I make soap. I make candles for family members. I’m by no means artistic, but I love being surrounded by it, and I love having it in my office. The students are really my favorite part of working at Otis.

